Dental implants serve as a reliable tooth replacement option for many people. Success rates exceed 90% in most cases, and implants can function well for many years with appropriate care.
However, dental implant fractures can occur in some situations. These complications remain uncommon, though understanding them remains valuable for informed decision-making. While eating with dental implants works well for most people, complications may arise over time.
Understanding what causes these fractures helps patients and dental professionals work together. This article examines the types of fractures that can occur, what contributes to them, and how they can be identified early. We also explore treatment approaches and prevention strategies.
Most implant issues can be addressed when identified promptly. Regular dental check-ups allow professionals to monitor implant health and detect potential concerns. For people eating with dental implants daily, knowledge about broken dental implant risk factors empowers informed decisions about dental care.
Contents Navigation
Summary of the Content
- Implant fractures involve three components: the crown, abutment/screw, or post, each requiring a specific treatment approach.
- Common implant fracture causes include grinding teeth, excessive force, narrow implant diameter, and bone loss.
- Warning signs include looseness, clicking during chewing, visible cracks, or bite changes that may require immediate evaluation.
- Diagnosis relies on clinical examination and X-rays or CBCT scans to locate fractures and assess fracture severity.
- Treatment ranges from crown replacement to full implant removal, depending on the fractured component.
- Prevention includes proper planning, night guards for grinders, good hygiene, and regular dental check-ups.
Understanding Dental Implant Components
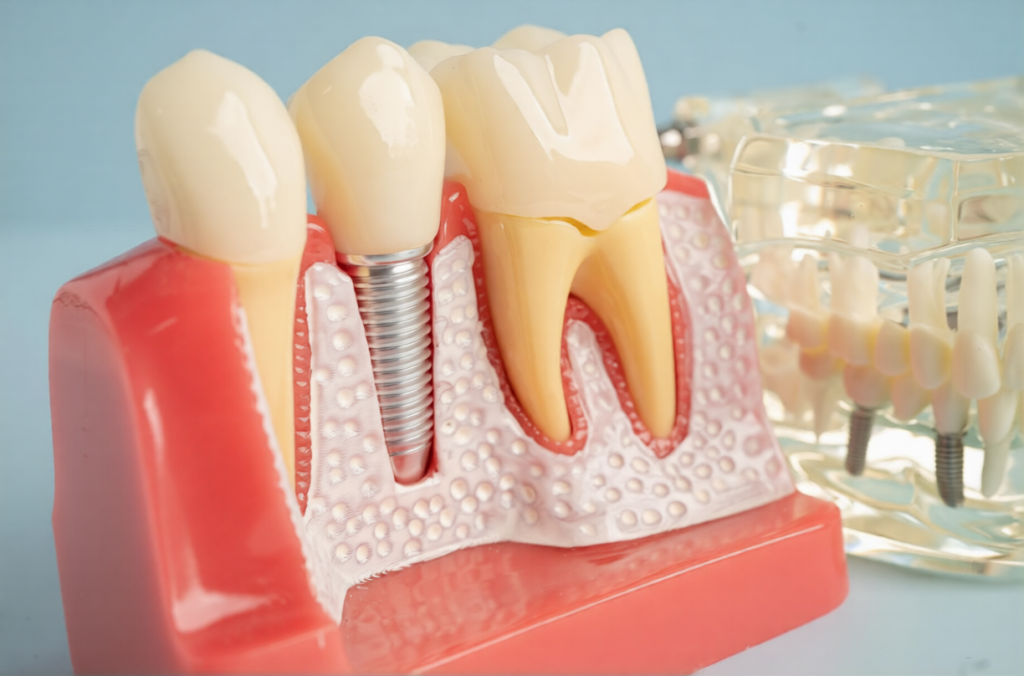
A dental implant consists of three main parts that work together as a functional unit.
The implant post, also called a fixture, is a titanium screw placed directly in the jawbone. This component serves as the artificial tooth root. Titanium offers biocompatibility, meaning the body accepts it without rejection. The post integrates with the surrounding bone through a process called osseointegration.
The abutment connects the implant post to the visible restoration. This component acts as a bridge between the two other parts. The abutment screws into the top of the implant post.
The crown represents the visible tooth restoration. Made from porcelain or zirconia, the crown matches the shape and colour of natural teeth. It attaches to the abutment and handles the forces of chewing.
These three components distribute chewing forces from the crown through the abutment to the implant post. The titanium post then transfers these forces to the surrounding jawbone. This system mimics how natural teeth and their roots function together.
Fractures can occur in any of these three components. The location of a fracture affects treatment options and outcomes. The abutment screw experiences considerable stress and ranks among the components most vulnerable to mechanical issues.
Osseointegration creates a direct connection between the titanium post and the jawbone. Unlike natural teeth, which have a periodontal ligament that cushions impact, implants lack this shock-absorbing layer. This rigid connection means forces are transferred directly to the implant components.
Types of Dental Implant Fractures
Different components of the implant system can fracture, each presenting distinct challenges.
- Crown Fractures
Crown fractures affect the visible part of the tooth restoration. Porcelain or zirconia can chip or crack under excessive force. These fractures often result from trauma or impact to the mouth.
Patients usually notice crown fractures immediately because they can see or feel the damage. The broken dental implant crown might have sharp edges or visible cracks. Treatment involves replacing the damaged crown while leaving the implant post and abutment intact. - Abutment and Screw Fractures
An implant screw fracture occurs when the abutment or its connecting screw breaks. This type ranks as the most common fracture affecting implant systems. Excessive load or loosening over time often contributes to these broken dental implant components.
Signs include a loose feeling in the crown or a clicking sensation when biting. The crown may appear to move slightly. Some people experience discomfort or sensitivity around the implant.
These implant screw fracture cases can be addressed without replacing the entire implant post. The damaged abutment or screw can be taken out, and a new one installed. A new crown may be needed depending on the extent of damage. - Implant Post Fractures
Fractures of the implant post itself represent the most serious type. These broken dental implant cases are rare but pose the most significant challenge. Post-fractures often develop after many years, sometimes a decade or more.
When a post fractures, the entire implant must be taken out. The area requires time to heal before replacement is considered. These fractures often occur gradually through metal fatigue rather than sudden trauma.
Common Causes of Dental Implant Fracture
Multiple factors can contribute to implant fractures. Many cases involve multiple risk factors rather than a single cause.
- Excessive Biting Forces
Implants can withstand normal chewing forces without difficulty. However, excessive or concentrated forces exceed the material tolerance of implant components. These excessive loads represent a primary implant fracture.
Biting forces concentrate on a single implant when insufficient implants support a restoration. Implant fracture causes often relate to this uneven force distribution. Non-balanced bite alignment creates uneven pressure across dental restorations.
Cantilever prostheses extend beyond the last supporting implant. This design creates a lever effect, multiplying forces at the implant connection point. Cantilever designs are known to significantly increase fracture risk. - Teeth Grinding and Clenching
Bruxism, the habit of grinding or clenching teeth, significantly increases the risk of implant complications. Studies indicate that people with bruxism face 2.2 to 4.7 times higher risk of implant issues compared to non-grinders.
Many people grind their teeth during sleep without awareness. This unconscious activity generates forces that exceed normal chewing pressures. The repetitive nature of grinding subjects implant components to cyclic loading over extended periods. This represents one of the most significant causes of broken dental implant complications in clinical settings. - Implant Diameter and Positioning
Implant diameter plays a crucial role in fracture resistance. Narrow implants measuring less than 3.5mm in diameter are associated with increased fracture risk, particularly in molar positions, where forces are greatest.
Molars and premolars handle the heaviest chewing forces in the mouth. Placing narrow implants in these high-stress locations creates a mismatch between force and structural strength. The implant may not have sufficient bulk to withstand the loads over time.
Research shows that 85% of implant fractures occur in the posterior regions, where chewing forces are concentrated. This makes implant positioning one of the key implant fracture causes. - Bone Loss and Infection
Progressive bone loss weakens the support structure around implants. As the bone recedes, it exposes weaker portions of the implant post. The remaining bone must bear all chewing forces on a smaller surface area.
Peri-implantitis, an inflammatory condition affecting tissues around implants, can lead to bone resorption. This infection-related bone loss compromises implant stability. The weakened support increases the likelihood of dental implant failure under normal loads. - Material Fatigue and Design
Metal fatigue develops through repeated loading cycles. Each chewing motion places stress on the implant material. After millions of cycles, microscopic cracks can develop and propagate. Preventing implant fracture requires attention to long-term material performance. - Prosthetic Factors
The design and fit of the crown or bridge affect the distribution of forces. An ill-fitting crown creates stress concentrations at connection points. A non-passive fit means the restoration doesn’t sit properly, creating internal strain even before chewing forces are applied.
Excessively wide crowns extend beyond the natural tooth dimension. This increases the surface area receiving biting forces. Cantilevers extending from attached bridges create leverage forces.
Signs and Symptoms to Watch For
Early recognition of implant problems allows for intervention before a complete fracture occurs.
- Early Indicators
Unusual mobility suggests loosening of implant components. A stable implant should not move or shift. Any sensation of looseness warrants professional evaluation.
Clicking or movement during chewing indicates that components aren’t fitting properly together. This sound or sensation often precedes visible damage. The abutment screw may be loosening before an implant screw fracture occurs.
Changes in bite alignment can signal implant problems. If the restoration suddenly feels high or different when biting, the implant system may have shifted.
Screw loosening often happens before an actual fracture. Regular check-ups allow dentists to identify and tighten loose screws before they break. - Visible Changes
A visible crack in the crown is a clear sign of damage. Even small chips or cracks can propagate under continued use. Any visible damage should be addressed promptly.
Changes in crown position suggest movement within the implant system. A crown that appears crooked or misaligned may indicate problems with the abutment or implant post.
A gap developing between the crown and gum tissue signals that something has shifted. The crown margin should fit closely against the gum line. - Inflammatory Signs
Spontaneous bleeding around an implant isn’t normal for healthy tissue. Bleeding may indicate inflammation or infection affecting the peri-implant area.
Swelling or inflammation around the implant suggests an active problem. The body responds to abnormal forces or movement with inflammation.
Tenderness on palpation of the area around an implant warrants evaluation. Healthy implants shouldn’t cause pain with light pressure. - Functional Changes
Difficulty chewing on the side with an implant suggests something isn’t working properly. People often unconsciously avoid using a restoration that doesn’t feel right.
Sounds when biting down can indicate loose or damaged components. Clicking, cracking, or popping noises during chewing aren’t normal.
A crown feeling high or misaligned affects chewing comfort. The restoration should blend seamlessly with the surrounding teeth.
Many fractures develop gradually without immediate symptoms. Regular professional check-ups remain important even when everything feels normal.
Diagnosis and Professional Evaluation
Accurate diagnosis guides appropriate treatment planning. Professional assessment combines multiple evaluation methods.
- Clinical Examination
Visual inspection of the implant and surrounding tissues is performed to identify obvious problems. Dentists look for cracks, gaps, swelling, or other visible changes.
Manual manipulation tests implant stability. Light pressure in different directions reveals any movement or looseness. Stable implants shouldn’t shift or rotate.
Bite assessment examines how the implant restoration meets opposing teeth. Uneven contact or high spots can contribute to excessive forces. - Imaging Methods
Periapical X-rays visualise the implant post and surrounding bone. These images show the bone level and any areas suggesting infection or bone loss. X-rays can sometimes reveal fracture lines in the post.
Panoramic radiographs provide a comprehensive view of all implants and jaw structures. This wide-angle image facilitates the simultaneous evaluation of multiple implants.
Cone-beam computed tomography (CBCT) scans provide detailed three-dimensional images. This advanced imaging reveals fractures not visible on standard X-rays. CBCT helps determine the exact fracture location and extent. - Diagnostic Process
Evaluation assesses the integrity of all three implant components. Dentists determine whether the crown, abutment, or post has damage.
Assessment of the surrounding bone evaluates the health of the support structure. Bone loss affects treatment planning and prognosis.
Assessing for signs of infection or peri-implantitis helps identify factors that may contribute to dental implant failure. Infection-related inflammation and bone loss must be addressed. Treatment aims to prevent further dental implant failure through comprehensive care.
Self-diagnosis cannot replace professional evaluation. Some fractures occur internally without external signs. Early detection through professional monitoring can prevent complications.
Treatment and Management Options
Treatment varies based on which component has fractured and the extent of damage.
- Crown Replacement
When the crown has fractured, but the implant post and abutment remain intact, crown replacement offers a straightforward approach. Digital impressions capture the precise position of the abutment. A new crown can be fabricated to match the surrounding teeth.
Temporary crowns may be provided while the final restoration is being made. The process involves taking out the damaged crown and assessing the abutment condition. - Abutment and Screw Replacement
When an implant screw fracture occurs, the damaged abutment or loose screw must be taken out. Special instruments allow this without damaging the implant post. The post is then evaluated for any damage or defects.
Installation of a new abutment and screw restores the connection between the post and the crown. The new abutment must fit precisely on the implant post.
This approach addresses the problem without requiring an implant post-extraction. The healing time is minimal compared to complete implant replacement. - Implant Post Fracture Management
Fractured implant posts require the extraction of the entire implant. Specific techniques help extract the fractured post while minimising bone damage.
The reverse torque technique works when the fractured portion remains accessible. The post is unscrewed in the opposite direction of installation. This method preserves the maximum amount of bone when successful.
Trephine bur methods cut around the implant post to free it from the surrounding bone. Small amounts of bone are taken out during this process.
Bone grafting may be necessary if significant bone loss occurs. Grafting material fills voids and provides a foundation for future implants. The graft requires time to heal before considering implant replacement.
A healing period allows tissues to recover after implant extraction. Bone requires time to regenerate before a new implant is placed. New implant placement can be considered after adequate healing. - Addressing Underlying Causes
Treatment must include addressing factors that contributed to the fracture. Bite adjustment helps distribute forces more evenly across all teeth.
Addressing grinding habits helps prevent future problems. Night guards protect implants from excessive forces during sleep. Occlusal splints distribute grinding forces across multiple teeth.
Infection control addresses peri-implantitis if present. Cleaning procedures clear bacterial deposits from implant surfaces. Preventing implant fracture includes maintaining healthy peri-implant tissues.
Prevention Strategies
Preventing dental implant complications proves more effective than managing them.
- Proper Planning and Placement
A comprehensive preoperative assessment evaluates bone quality and quantity. Three-dimensional imaging provides precise measurements of bone dimensions and density.
An adequate implant diameter for the location reduces fracture risk. Molars require larger diameter implants than front teeth. A minimum diameter of 3.5mm is recommended, with larger sizes for high-stress areas.
Sufficient implants to support the planned restoration distribute forces appropriately. Planning accounts for expected force levels. - Managing Grinding Habits
Night guards help people with bruxism protect their implants. Custom-fitted guards distribute grinding forces across all teeth. This reduces the concentration of stress on individual implants.
Occlusal splints serve a similar protective function. These devices prevent direct tooth-to-tooth contact during grinding episodes.
Stress-related grinding management addresses root causes. Increased implant numbers for bruxism patients provide additional support. More implants mean each one bears less individual load. - Prosthetic Design Considerations
Proper crown fit and occlusion reduce stress concentrations. Crowns should fit accurately without gaps or high spots. A passive fit means there is no internal strain when the crown is placed.
Minimising cantilevers, where possible, reduces leveraged forces. When cantilevers are necessary, keeping them short limits the multiplication of forces.
Appropriate occlusal table size keeps forces within manageable limits. Crown width should match natural tooth dimensions.
Balanced occlusion distributes forces evenly across all teeth. No single tooth should contact significantly before the others. - Regular Professional Maintenance
Routine dental examinations monitor the health of dental implants over time. Regular check-ups allow early detection of loosening or problems. Many issues can be addressed before they progress to fractures.
Early intervention addresses problems in their initial stages. Tightening a loose screw takes minutes and prevents more serious issues.
Professional cleaning prevents peri-implantitis development. Bacterial accumulation around implants can lead to inflammation and bone loss.
Periodic imaging assesses bone levels around implants. X-rays show bone changes that aren’t visible during clinical examination. - Patient Self-Care
Thorough oral hygiene practices maintain healthy tissues around implants. Brushing and flossing clear bacterial deposits. Clean implants are less likely to develop peri-implantitis.
Avoiding extremely hard foods protects implants from excessive force. Ice, hard lollies, and bones can generate forces exceeding implant tolerance.
Not using teeth as tools prevents trauma to implants. Using teeth to open items or biting fingernails subjects teeth to abnormal forces.
Protecting implants during contact sports prevents traumatic damage. Mouthguards cushion impacts during physical activities.
Following postoperative care instructions supports proper healing. Compliance with recommendations reduces the risk of early complications. - Managing Bone Health
Maintaining peri-implant hygiene prevents peri-implantitis and preserves bone support. Healthy bone provides the foundation for long-term implant success.
Addressing bone loss promptly limits its extent. Early treatment of peri-implantitis can halt progression. Some bone regeneration may occur with appropriate therapy.
Managing conditions affecting bone health supports implant longevity. Diabetes control, osteoporosis management, and adequate nutrition all influence bone quality. - Lifestyle Factors
Smoking cessation improves bone health and healing. Smoking affects blood flow to bone tissue, compromising osseointegration.
Managing systemic health conditions supports overall healing capacity. Well-controlled diabetes, hypertension, and other conditions improve treatment outcomes.
Adequate nutrition provides building blocks for bone health. Calcium, vitamin D, and protein support bone maintenance.
Preventing implant fracture requires attention to multiple factors. No single strategy eliminates all risk, but combining approaches reduces the likelihood of complications.
When to Seek Professional Care
Knowing when to contact your dental professional enables timely intervention.
- Immediate Attention Situations
Visible crown breakage or fracture requires prompt care. Broken pieces should be saved in a clean container and brought to the appointment. Sudden looseness or mobility of an implant warrants immediate evaluation. Implants should remain stable and immovable.
Significant pain or swelling around an implant needs urgent assessment. Severe symptoms might indicate infection or mechanical issues. An implant that has fallen out completely requires immediate attention. Trauma to the mouth involving an implant needs evaluation. - Schedule Prompt Appointment
Unusual clicking or movement during chewing should be evaluated soon. These sounds often indicate loosening before visible damage occurs. Minor discomfort or sensitivity around an implant warrants attention. Scheduling an appointment within a few days is appropriate.
Changes in bite alignment need professional evaluation. Bleeding around an implant should be assessed. Any concerns about implant integrity deserve attention. Trust your instincts if something feels wrong. - Regular Monitoring
Routine check-ups remain important even in the absence of symptoms. Many problems develop gradually without obvious signs. Professional cleaning appointments maintain tissue health. These appointments often include brief implant assessments. - Before Your Appointment
Keep any broken pieces in a clean container. Avoid chewing on the affected side until evaluation. Maintain careful oral hygiene around the affected area. Use a cold compress if swelling occurs.
Don’t attempt DIY approaches or temporary measures. Early professional assessment of implant problems often allows simpler treatment.
Final Thoughts
Dental implant fractures occur in a small percentage of cases. Most implants function well for many years without complications. Eating with dental implants usually works successfully when proper care is maintained. Different fracture types require varying treatment approaches. Crown fractures require straightforward replacement, whereas post fractures require complete implant extraction.
Multiple factors can contribute to fracture risk. Excessive forces, grinding habits, inadequate planning, and bone loss all play roles. Most cases involve a combination of factors. Prevention strategies can reduce the likelihood. Proper planning, addressing grinding habits, regular monitoring, and thorough hygiene all support long-term success.
Regular dental check-ups allow monitoring of implant health. Professional evaluation can detect early warning signs before major problems develop. Professional guidance is available when concerns arise. Dental professionals can evaluate symptoms, provide an accurate diagnosis, and recommend appropriate treatment.
Dental implants remain a highly successful treatment option for replacing missing teeth. The majority of patients experience no fracture complications. With proper care and monitoring, implants can serve well for many years.
Knowledge empowers informed decision-making about dental care. The partnership between patient and dental professional supports the goal of long-term implant success.
If you have concerns about your dental implants or questions about how to prevent complications, contact your dental professional. They can provide personalised guidance based on your specific situation and health history.
Important Information
Any surgical or invasive procedure carries risks. Before proceeding, you should seek a second opinion from an appropriately qualified health practitioner.
A consultation is required to assess your individual circumstances. Results may vary among patients due to multiple factors.
This information is provided for educational purposes. It should not replace professional dental advice. Consult with a qualified dental professional about your specific situation.