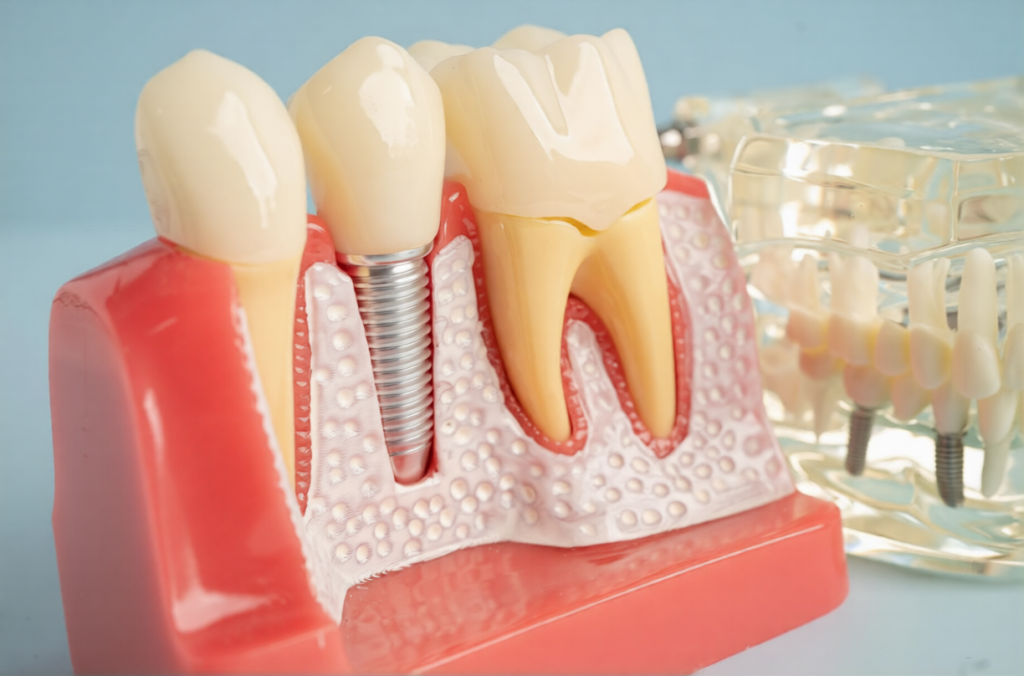
Dental implants offer a long-term tooth replacement option with success rates exceeding 90%. This high success rate reflects the durability of implants when properly maintained. However, peri-implantitis can affect 5-8% of dental implants over time, making awareness and prevention essential for protecting your implants.
Peri-implantitis is an inflammatory condition affecting the tissues surrounding dental implants. Early detection and preventive care can help protect implant health and function. Understanding the warning signs may support timely professional care when needed.
This guide provides evidence-based information to help you understand peri-implantitis and support long-term implant health. We cover what peri-implantitis is, how it develops, the symptoms to watch for, and how professional care can help address it.
- Peri-implantitis involves bone loss around dental implants caused by bacterial plaque buildup, distinguishing it from simpler gum inflammation.
- The condition differs from peri-implant mucositis, which affects only soft tissue and does not involve bone, and can be reversed with care.
- Research indicates 5-8% of dental implants may be affected by peri-implantitis over time, with risk increasing 5-10 years after placement.
- Risk factors include a history of gum disease, inadequate oral hygiene, smoking, poorly controlled diabetes, and lack of regular professional monitoring.
- Early symptoms of peri-implantitis often include bleeding around the implant and swollen gums, whilst advanced cases may involve loose crowns, discomfort, or visible pus.
- Preventing implant failure focuses on daily home care, professional dental implant maintenance visits every 3-6 months, and lifestyle factors like smoking cessation.
- Treatment approaches for dental implant infection range from non-surgical cleaning and antiseptic therapy to surgical intervention, depending on disease severity.
- Regular professional monitoring can help detect issues before they progress to advanced stages.
Understanding Peri-Implantitis: More Than Just Gum Inflammation
Peri-implantitis is an inflammatory condition affecting the tissues around dental implants. Bacterial plaque buildup triggers this condition, leading to progressive changes in the supporting structures. The key characteristic that distinguishes peri-implantitis from simpler inflammation is the presence of bone loss around the implant.
Dental implants differ from natural teeth in important ways. Natural teeth have a periodontal ligament that helps protect against bacterial invasion. Implants lack this protective structure, which can make the surrounding tissues more vulnerable to bacterial infection when plaque accumulates.
Peri-Implant Mucositis vs Peri-Implantitis
Understanding the difference between these two conditions can help you recognise when to seek professional care. Peri-implant mucositis involves only soft-tissue inflammation and can be reversed with appropriate care. Think of mucositis as an early warning system, similar to gingivitis around natural teeth.
Peri-implantitis involves bone loss in addition to soft tissue inflammation. Once bone loss occurs, the damage cannot be reversed, though progression can often be halted with appropriate care. This makes early detection particularly important for long-term implant health.
How Common is Peri-Implantitis?
Research shows that peri-implantitis affects 5-8% of dental implants over time. The risk tends to increase with time, with cases most commonly appearing 5-10 years after implant placement. Individual risk varies based on many factors, including oral hygiene habits, smoking status, and overall health conditions.
Causes and Risk Factors
The primary cause of peri-implantitis is bacterial biofilm accumulation around the implant. Gram-negative anaerobic bacteria, similar to those involved in gum disease, colonise the implant surface and surrounding tissues. The presence of chronic bacteria triggers an inflammatory response in the body. Over time, this inflammation breaks down the bone supporting the implant.
Patient Risk Factors
Several factors can increase the likelihood of developing peri-implantitis:
Strong Evidence:
- Gum Disease History:
A history of gum disease indicates that similar bacterial susceptibility may affect implants. - Inadequate Oral Hygiene:
Plaque can accumulate around implant restorations. - Smoking:
Smoking significantly increases risk and impairs the body’s healing response. - Poorly Controlled Diabetes:
Poorly controlled diabetes impairs immune function and tissue healing. - Lack of Maintenance:
Regular professional maintenance can help detect early problems.
Moderate Evidence:
- Genetic Factors:
Genetic factors may affect an individual’s immune response to bacteria. - Certain Medications:
Certain medications can influence immune function and tissue health. - Heavy Alcohol Use:
Heavy alcohol consumption may impact oral health and healing. - Nutritional Deficiencies:
Nutritional deficiencies can affect tissue maintenance and healing.
Implant-Related Factors
Certain characteristics of the implant and restoration may influence the risk of peri-implantitis. Implant surface roughness helps initial bone integration, but can provide areas where bacteria may accumulate. Excess cement from the restoration, if not removed completely during placement, can harbour bacteria. A prosthetic design that limits access for cleaning can make adequate home care challenging. Implant position may affect how easily you can clean around the restoration.
These factors represent general clinical considerations rather than issues with any particular dental clinic’s work. Regular professional monitoring can help identify and address these concerns before they escalate.
Warning Signs
Early detection allows for more conservative care approaches. Many symptoms of peri-implantitis can be detected during professional dental examinations before you notice changes at home.
What Your Dentist May Detect
During routine examinations, your dentist checks for several indicators of peri-implant health:
- Bleeding when lightly probing around the implant can signal inflammation.
- Increased pocket depth, measured during exams, may indicate tissue changes.
- Visible bone loss on X-rays provides important information about implant support.
- Pus or suppuration around the implant indicates active dental implant infection.
What Patients May Notice
Early Signs:
You might observe these early symptoms of peri-implantitis at home:
- Swollen, red, or tender gums around the implant restoration indicate inflammation.
- Bleeding when brushing or flossing around the implant, particularly when this didn’t occur previously, warrants attention.
- Mild sensitivity around the implant site may develop.
- The gum pulling away from the crown can become visible.
Advanced Signs:
These symptoms typically develop as the condition progresses:
- Persistent bad taste or odour around the implant suggests ongoing infection.
- Visible pus indicates an active dental implant infection requiring prompt care.
- The implant crown may feel loose or shift slightly.
- Changes in how your teeth come together when you bite can occur.
- Discomfort when chewing may develop as the condition advances.
Peri-implantitis often doesn’t cause pain in the early stages. Discomfort usually appears only during acute infection phases. This is why you shouldn’t wait for pain before seeking professional evaluation of any changes around your implant.
When to Contact Your Dentist
Several signs indicate you should schedule an appointment for professional evaluation:
- Any bleeding around the implant when this wasn’t occurring previously deserves attention.
- Swelling or redness lasting more than a few days should be assessed.
- Changes in how the crown fits or feels require professional examination.
- Any discharge or pus around the implant needs prompt evaluation.
- New sensitivity around the implant site warrants a professional assessment.
Prevention Strategies
Preventing implant failure requires consistent daily care combined with regular professional monitoring. Implants need cleaning just as carefully as natural teeth. Many patients mistakenly believe that because implants can’t develop cavities, they need less care. The surrounding tissues can become infected, making thorough dental implant maintenance essential.
Daily Home Care
Taking care of your implant at home involves three key components that work together to maintain implant health.
Brushing Technique
Proper brushing forms the foundation of implant care. Brush at least twice daily using a soft-bristled brush, paying close attention to where the crown meets the gum line. Use gentle circular motions rather than aggressive scrubbing, which can irritate tissues. Electric toothbrushes can be effective when used properly. Replace your brush every three months to maintain cleaning effectiveness.
Flossing and Interdental Cleaning
Daily flossing or interdental brush use is essential for implant health. Customised implant floss is available and may be recommended by your dentist. Water flossers can complement traditional floss but shouldn’t replace it entirely. Make sure to clean all sides of the implant restoration thoroughly each day.
Antimicrobial Rinses
These may be recommended as an additional care measure to support gum health around your implant. Chlorhexidine or prescribed rinses are typically for short-term use rather than daily long-term application. Ask your dentist about appropriate products for your specific situation.
Implants need cleaning just like natural teeth. Many patients think “can’t get cavities equals less care needed”—this is a misconception. The surrounding tissues can become infected, making daily care essential for preventing implant failure.
Professional Maintenance
Regular professional care plays a crucial role in protecting implant health and detecting problems early.
Recommended Visit Schedule:
- First Year Monitoring:
During the first year after implant placement, visits every 3-4 months allow your dentist to closely monitor healing and integration. - Ongoing Maintenance:
After the first year, visits every six months are typically recommended for healthy implants with no complications. - High-Risk Patients:
If you have risk factors like smoking or diabetes, more frequent appointments may benefit your long-term outcomes.
What Happens During Your Maintenance Visit
Your dental implant maintenance appointment includes several important checks. Your dentist performs a visual examination of the soft tissue around the implant, looking for signs of inflammation or changes. Probing depths are measured and compared to your baseline measurements to detect any changes early. The area is checked for bleeding when carefully probed, which can indicate inflammation. Periodic X-rays, typically taken annually, show bone levels around the implant and help identify any bone loss. Professional cleaning uses specific instruments specifically designed for implant surfaces that won’t scratch or damage the implant.
Lifestyle Factors
Beyond daily care and professional visits, certain lifestyle choices significantly impact implant health.
| Factor | Impact on Implant Health | What You Can Do |
| Smoking | Most significant modifiable risk factor for peri-implantitis; slows healing and increases infection risk | Quitting improves outcomes; your dentist can provide cessation resources and support |
| Diabetes | Poorly controlled blood sugar increases infection risk and affects tissue healing | Work with your physician for optimal control; well-managed diabetes reduces peri-implantitis risk |
| Nutrition | Adequate vitamins and minerals support tissue health and bone maintenance | Maintain sufficient vitamin D and calcium intake through diet or supplements |
| Teeth Grinding | Excessive forces can stress implants and the surrounding bone | Custom night guard protects both implants and natural teeth from grinding damage |
| Stress | May impact immune function and overall oral health | Stress management techniques may help support immune function |
These lifestyle factors work together with your daily care routine and professional maintenance to support long-term implant success and help prevent implant failure.
How Diagnosis is Made
Diagnosis of peri-implantitis involves a clinical examination and radiographic assessment.
Clinical Examination
Your dentist performs a visual inspection to assess tissue colour, swelling, and texture around the implant. Probing pocket depths around the implant are measured and recorded. The area is checked for bleeding when gently probed. The implant is assessed for any mobility. Healthy implants should be completely stable.
Radiographic Assessment
Periapical X-rays show bone levels around the implant. These images are compared to baseline radiographs from placement to identify any bone loss. Progressive bone loss on serial X-rays over time indicates active disease. CBCT (cone beam computed tomography) provides three-dimensional imaging when needed for complex cases.
Key Indicators
Several findings indicate peri-implantitis may be present. Bone loss exceeding 2mm from baseline after the first year suggests possible problems. Progressive loss visible on serial X-rays indicates active disease. Crater-shaped bone defects around the implant are characteristic patterns.
Distinguishing From Other Conditions
Your dentist differentiates peri-implantitis from several similar conditions. Peri-implant mucositis involves inflammation without bone loss. Occlusal overload results from excessive biting forces and shows different patterns. Cement-related inflammation can occur if excess cement remains from restoration placement. Failed osseointegration represents early implant failure with characteristics distinct from those of peri-implantitis.
Treatment Options
Treatment approaches for peri-implantitis depend on disease severity and individual circumstances. Care aims to halt disease progression, reduce inflammation, and, where possible, support long-term implant function.
Non-Surgical Treatment (Early Disease)
- Professional Mechanical Debridement
Thorough removal of plaque and calculus around the implant represents the foundation of care. Tailored instruments made of carbon fibre or plastic are used to avoid scratching the implant surface. Metal instruments could damage the implant, so careful selection of cleaning tools is important. Several appointments may be needed for comprehensive cleaning.
Research shows this approach can provide short-term improvement, though it may not be sufficient alone for controlling the condition in all cases. - Antiseptic Therapy
Chlorhexidine rinses or gels may be used as part of the care approach. These can be applied below the gum line during professional appointments. Daily rinses for 3-4 weeks are typically recommended. Temporary tooth staining can occur but is removable. - Antibiotic Therapy
When appropriate as part of a comprehensive approach, antibiotics may be considered. These can be taken systemically (pills) or applied locally to the affected area. Antibiotic selection targets anaerobic bacteria commonly involved in the condition. The usual duration of systemic antibiotics is 7-10 days when prescribed. Antibiotics are not routinely used as first-line care but may be included based on individual assessment. - Laser-Assisted Therapy
Diode or CO₂ lasers can be used for surface decontamination. This approach may support soft tissue healing in some cases. Research shows mixed results regarding the effectiveness of laser therapy. Laser treatment is usually combined with other care approaches.
Surgical Treatment (Advanced Disease)
Surgical approaches may be considered when non-surgical methods haven’t achieved adequate results or when bone loss is moderate to advanced.
When Surgical Approaches May Be Indicated:
- Moderate to advanced bone loss around the implant
- Persistent infection despite non-surgical care
- Deep pockets that cannot be adequately cleaned without surgical access
Types of Surgical Approaches:
- Access Flap Surgery
The soft tissue is carefully lifted to expose the implant surface. This allows direct access for thorough cleaning and decontamination. Infected tissue can be removed during the procedure. The implant surface is decontaminated using appropriate methods. Tissue is repositioned and sutured after cleaning. - Resective Surgery
This approach reshapes bone to eliminate deep pockets around the implant. The goal is to create shallower, more maintainable pocket depths. Some additional bone may be removed to achieve proper contours. This can make ongoing home care and professional cleaning more effective. - Regenerative Surgery
This approach attempts to rebuild lost bone around the implant. Bone grafting materials may be placed to support regeneration. Barrier membranes can guide tissue regeneration. Success varies depending on defect type, with crater-shaped defects showing better potential for regeneration than other patterns.
Implant Removal
In some situations, implant removal may be necessary.
When Removal May Be Considered:
- Severe bone loss compromising implant stability
- Progressive disease despite appropriate care attempts
- Implant mobility indicates loss of support
- Persistent infection that doesn’t respond to other approaches
The Removal and Potential Replacement Process:
The implant is carefully removed while preserving as much bone as possible. A healing period of 3-6 months typically follows removal. Bone grafting may be needed to restore adequate bone volume. Re-implantation may be possible after complete healing, depending on individual circumstances.
Treatment Decision-Making
Care approaches are individualised based on each patient’s specific situation. A staged approach often works well, starting with non-surgical care, then reassessing results and considering surgical options if needed. Decisions involve discussion between the patient and dentist about realistic expectations and preferred approaches.
Results vary between individuals. Treatment outcomes can’t be certain. Individual factors determine the success of different approaches.
Long-Term Management
Aftercare for peri-implantitis, along with ongoing monitoring and maintenance, becomes even more important.
Ongoing Maintenance
More frequent monitoring is typically recommended after peri-implantitis care, often every 3-4 months. Continued diligent home care remains essential for maintaining results. Regular probing and X-rays help track tissue response and stability. Care protocols may be adjusted based on how tissues respond over time.
Realistic Expectations
The goal of care is to achieve stable, maintainable tissues around the implant. Complete bone regeneration to pre-disease levels is rarely achieved. Halting the progression of the condition can be considered a successful outcome. Some implants that have been addressed for peri-implantitis can remain functional for years with proper ongoing maintenance.
Prognosis Factors
Several factors can influence long-term outcomes. The severity of bone loss at the time care begins affects potential results. Patient compliance with ongoing maintenance visits is crucial. Control of risk factors, particularly smoking cessation and diabetes management, influences outcomes. The quality of daily home care affects long-term tissue health. Regular professional monitoring helps detect any changes early.
Some implants may require removal despite care efforts. Care approaches aim to preserve implants when possible, though this is not always possible.
If Initial Care Doesn’t Achieve Desired Results
In some cases, repeat care may be considered if initial approaches don’t achieve stable tissue health. Implant removal and discussion of alternative tooth-replacement options may be necessary. Individual assessment guides decisions about next steps. Options after implant removal can include placement of a different implant after healing, a dental bridge, or a partial denture, depending on your specific situation.
Choosing Experienced Care
Experience with dental implant care and monitoring supports the proper assessment. Appropriate diagnostic tools, including quality X-ray equipment, support accurate evaluation. Customised cleaning protocols and implant instruments are important for proper maintenance. A comprehensive monitoring system helps track implant health over time.
Final Thoughts
Peri-implantitis is a serious condition affecting the tissues and bone around dental implants. However, this condition is largely preventable through consistent daily care and regular professional dental implant maintenance. Early detection of symptoms of peri-implantitis allows for more conservative care approaches before significant bone loss occurs. Both home care and professional monitoring work together to maintain implant health over time.
Several key practices support long-term implant health. Maintain diligent daily hygiene around your implants, including thorough brushing and interdental cleaning. Professional appointments provide essential monitoring and thorough cleaning that you cannot achieve at home. Contact your dentist promptly if you notice warning signs such as bleeding, swelling, or changes around your implant. If you smoke, consider smoking cessation to reduce your risk significantly. Stay committed to long-term care, as preventing implant failure requires ongoing attention throughout the functional life of your implants.
Professional implant care is available at our Adelaide dental clinic. My Dentist Blackwood welcomes patients with dental implants for maintenance and assessment. Contact our team to discuss your implant health and any concerns. With proper care and attention, dental implants can function successfully for many years. Understanding peri-implantitis and its prevention can support the long-term success of your implant investment.